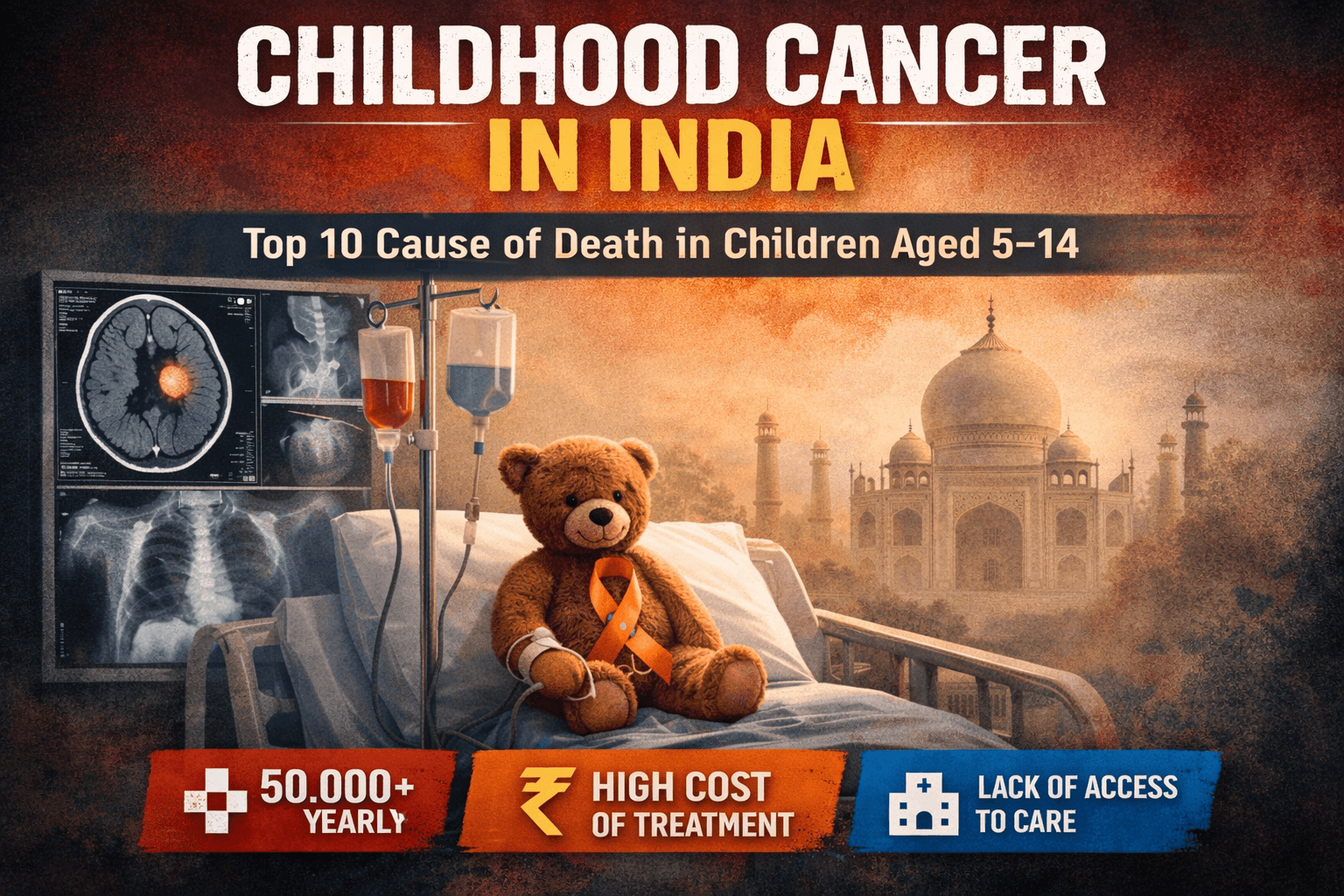Childhood Cancer in India: A Concerning Rise as It Becomes a Leading Cause of Death Among Children
Cancer is increasingly emerging as a significant public health concern among children in India. According to recent research highlighted by Indian Express, cancer has now entered the top 10 causes of death among children aged 5–14 years in India.
This marks a critical shift in India’s child health landscape, where infectious diseases and malnutrition have traditionally been the dominant causes of mortality. The growing burden of childhood cancer reflects both improved detection and deeper systemic challenges in healthcare access and early diagnosis.
What the Study Actually Says
The report referenced by Indian Express is based on findings published in a peer-reviewed medical journal, which analyzed long-term mortality trends in India.
Key verified takeaways:
- Cancer is among the top 10 causes of death in children aged 5–14 years in India
- It is not the single leading cause, but a significant contributor
- The rise is linked to epidemiological transition and better diagnosis/reporting
This is consistent with global patterns reported by the World Health Organization, which states that cancer is a leading cause of death among children worldwide, though rankings vary by country.
Understanding Childhood Cancer in India
Childhood cancer refers to cancers occurring in individuals under the age of 15. Unlike adult cancers, these are rarely linked to lifestyle and are often caused by genetic or developmental factors.
In India, the burden is substantial due to the country’s large population.
Verified Data Points
- India reports approximately 50,000–60,000 new childhood cancer cases annually
- Childhood cancers account for about 3–4% of total cancer cases in India
- India contributes a significant share of global childhood cancer cases, though exact percentages vary by study
These estimates are supported by data from institutions such as the Indian Council of Medical Research and hospital-based cancer registries.
Most Common Types of Childhood Cancer
The types of cancer affecting children differ significantly from those seen in adults.
Common Pediatric Cancers in India
- Leukaemia (blood cancer) – most common
- Brain and central nervous system tumours
- Lymphomas
- Neuroblastoma
- Wilms’ tumour (kidney cancer)
- Bone cancers (osteosarcoma, Ewing sarcoma)
These cancers often develop rapidly but are also highly treatable if detected early.
Why Is Childhood Cancer Becoming More Visible?
The increase in reported childhood cancer cases does not necessarily mean the disease itself is rising dramatically. Instead, multiple factors are contributing to its growing visibility:
1. Improved Diagnosis and Reporting
Expansion of cancer registries and better diagnostic tools have led to more accurate identification of cases.
2. Decline in Infectious Disease Mortality
As deaths from infections decrease, non-communicable diseases like cancer become more prominent in mortality rankings.
3. Population Size
India has one of the largest child populations globally, which increases the absolute number of cases.
4. Increased Awareness
More families are now seeking medical care, leading to better detection.
The Real Challenge: Late Diagnosis
One of the most critical issues in India is delayed diagnosis of childhood cancer.
Common Reasons
- Symptoms like fever or fatigue are often mistaken for infections
- Limited awareness among parents and primary healthcare providers
- Lack of specialized pediatric oncology services in rural areas
- Delays in referral systems
Because of these delays, many children are diagnosed at advanced stages, reducing survival chances.
Survival Rates: India vs Developed Countries (Fact-Checked)
There is a significant disparity in survival outcomes:
- High-income countries: 80–90% survival rates for many childhood cancers
- India: Survival rates vary widely, often estimated between 50–70% in better centers, but significantly lower in underserved regions
The World Health Organization highlights that most childhood cancers are curable with timely treatment, making early diagnosis crucial.
Read more on Change in CBSE Curriculum.
Barriers to Treatment in India
1. Unequal Access to Healthcare
Advanced cancer treatment facilities are concentrated in urban areas.
2. Financial Burden
Cancer treatment can be expensive, and many families lack insurance coverage.
3. Treatment Abandonment
Some families discontinue treatment due to cost, travel challenges, or lack of support.
4. Awareness Gap
Early warning signs are often overlooked.
5. Social Factors
In some cases, gender disparities influence access to care.
Why This Matters: A Changing Health Landscape
The inclusion of cancer among the top causes of child mortality signals a broader shift:
- India is transitioning toward non-communicable diseases
- Child health policies must evolve accordingly
- Healthcare systems need to adapt to long-term disease management
This trend does not replace traditional concerns like malnutrition—but adds a new layer of complexity.
Government and Policy Response
India has taken several steps to address cancer care:
- National Cancer Registry Programme (NCRP)
- Ayushman Bharat for financial support
- Expansion of cancer treatment centers
However, experts note that childhood cancer requires more focused policy attention, including:
- Dedicated pediatric oncology programs
- Nationwide awareness campaigns
- Strengthening referral systems
What Needs to Be Done Next
1. Early Detection and Awareness
Training frontline healthcare workers to identify symptoms can save lives.
2. Expanding Treatment Access
More pediatric oncology centers are needed beyond major cities.
3. Financial Protection for Families
Reducing out-of-pocket expenses can prevent treatment dropout.
4. Data and Research
Better national data will help design targeted interventions.
5. Community-Level Education
Parents must be aware of early warning signs such as:
- Persistent fever
- Unexplained weight loss
- Swelling or lumps
- Fatigue
The Reality: A Treatable Yet Overlooked Crisis
Childhood cancer is not always preventable, but it is often treatable and even curable. The biggest barrier in India is not medical capability—but timely access to care.
The fact that cancer is now among the top 10 causes of death in children should be seen as a call to action.
Conclusion
The rise of childhood cancer in India as a leading cause of death among children reflects a changing health landscape. While improved diagnosis has brought greater visibility, it has also exposed critical gaps in healthcare access, awareness, and affordability.
Addressing this challenge requires coordinated efforts from policymakers, healthcare providers, and society. With the right interventions—especially early diagnosis and accessible treatment—many young lives can be saved.
India now stands at a crucial point where childhood cancer must become a national health priority.